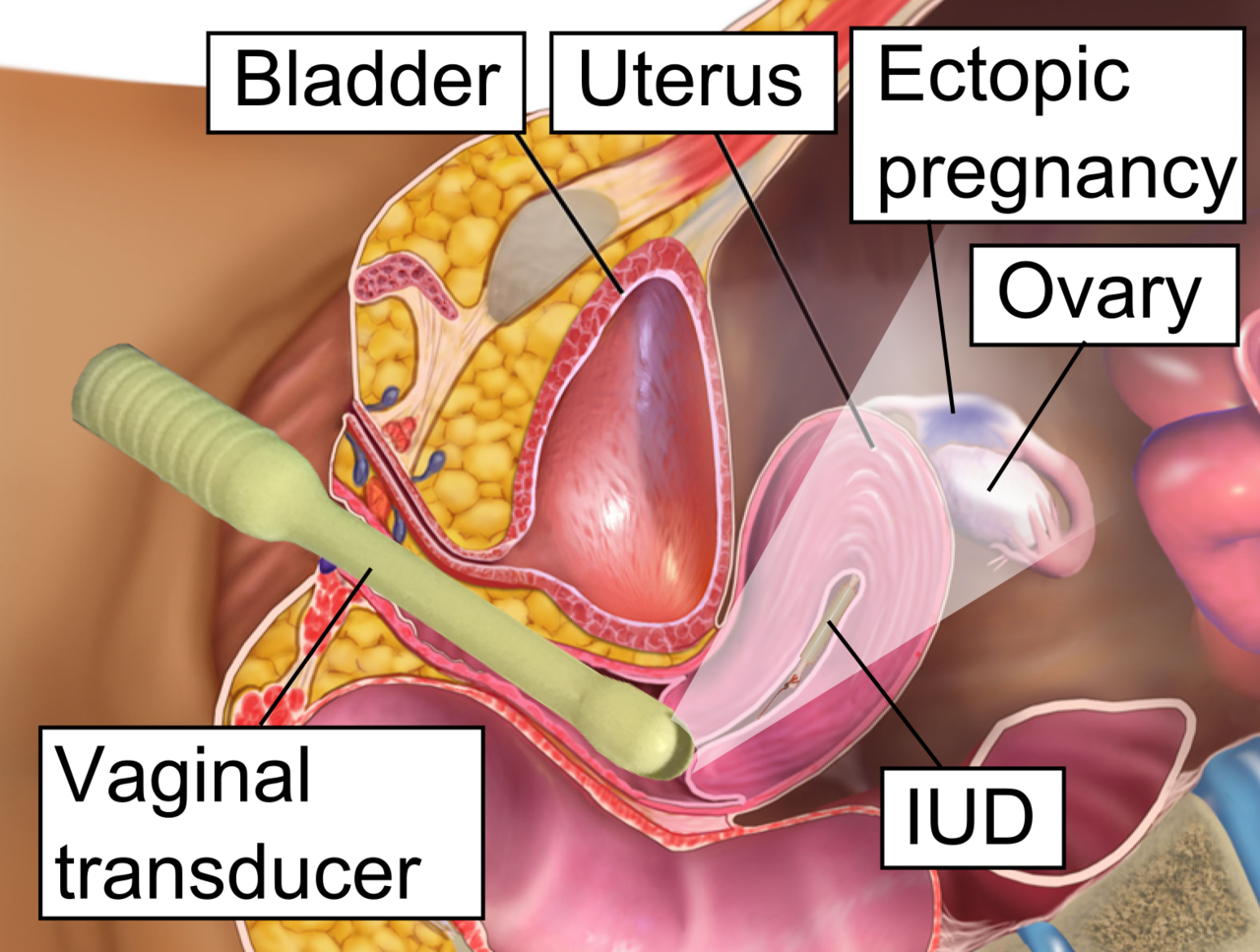
An ectopic pregnancy is a condition where the fertilized egg implants and grows outside the uterus, typically in the fallopian tube. This type of pregnancy is not viable, meaning the embryo cannot survive and develop normally. It poses a significant risk to the health of the mother if left untreated.
In cases of ectopic pregnancy, the fallopian tube containing the ectopic pregnancy can rupture, leading to internal bleeding in the abdomen. This can result in a life-threatening condition called hemorrhagic shock. Therefore, prompt medical intervention is crucial.
Laparoscopy, a minimally invasive surgical technique, is commonly used to manage ectopic pregnancies. It offers several advantages, including smaller incisions, reduced blood loss, shorter hospital stays, faster recovery times, and lower risk of complications compared to traditional open surgery.
During laparoscopic intervention for ectopic pregnancy, the surgeon assesses the extent of the condition and determines the most appropriate course of action. In some cases, the affected fallopian tube may need to be removed (salpingectomy) if it is severely damaged or ruptured. Alternatively, if the tube is relatively intact, the ectopic sac may be removed while preserving the tube (salpingostomy). The decision is based on the individual patient's condition and the surgeon's judgment.
By utilizing laparoscopy, the surgical team can carefully access and treat the ectopic pregnancy, minimizing trauma to surrounding tissues and reducing the risk of complications. Following the procedure, patients are closely monitored for recovery, and additional medical management may be provided as needed.
Laparoscopy has become an integral part of the surgical management of various malignancies affecting the ovaries, uterus, and cervix. This minimally invasive surgical technique offers numerous advantages over traditional laparotomy procedures. With advancements in technology and surgical skills, many surgeries that were previously performed through open surgery can now be effectively managed through laparoscopy.
For malignancies involving the ovaries, laparoscopy enables the surgeon to perform procedures such as ovarian cystectomy, oophorectomy (removal of the ovary), or even staging procedures for ovarian cancer. In cases of uterine malignancies, laparoscopy allows for total hysterectomy, bilateral salpingo-oophorectomy, and lymph node dissection. Furthermore, for cervical malignancies, radical hysterectomy and lymphadenectomy can be accomplished through laparoscopy.
The benefits of laparoscopy in malignancy management are substantial. By accessing the surgical site through small incisions, laparoscopy reduces surgical trauma, resulting in less post-operative pain, decreased blood loss, and reduced hospital stays. Additionally, laparoscopy offers enhanced visualization, allowing for meticulous dissection and precise surgical techniques. These advantages collectively contribute to a lower morbidity rate, faster recovery, and improved patient outcomes.
It is important to note that not all malignancies are suitable for laparoscopic management, and the decision for the surgical approach should be based on various factors, including the stage and extent of the malignancy, the patient's overall health, and the surgeon's expertise. Consultation with a qualified gynecologic oncologist or surgical specialist is essential to determine the most appropriate treatment approach for each individual case.
The procedure for laparoscopy in the management of malignancies involving the ovaries, uterus, and cervix typically involves the following steps:
- Anesthesia: You will be given anesthesia to ensure that you are comfortable and pain-free during the surgery. The type of anesthesia used may vary, and your healthcare team will discuss this with you beforehand.
- Port Placement: Small incisions, usually around 0.5 to 1 centimeter in size, are made in the abdominal wall. These serve as entry points for the laparoscopic instruments and the camera.
- Creation of Pneumoperitoneum: Carbon dioxide gas is introduced into the abdominal cavity to create a pneumoperitoneum. This helps to create space for visualization and manipulation of the organs during the procedure.
- Insertion of Laparoscope: A laparoscope, which is a thin, lighted tube with a camera at the end, is inserted through one of the incisions. The camera provides a magnified view of the internal organs on a monitor, allowing the surgeon to perform the procedure with precision.
- Instrument Insertion and Surgical Manipulation: Additional specialized instruments are inserted through the other incisions. These instruments allow the surgeon to perform various surgical tasks, such as tissue dissection, cutting, suturing, and removal of tissue samples for biopsy.
- Tumor Management: The specific steps involved in tumor management depend on the nature and extent of the malignancy. For example, in cases of ovarian cancer, the surgeon may perform tumor debulking, removal of affected ovaries, or staging procedures. In uterine or cervical malignancies, the surgeon may proceed with total hysterectomy, removal of nearby lymph nodes, and other necessary procedures.
- Wound Closure: After the tumor management is completed, the instruments are removed, and the gas is released from the abdominal cavity. The small incisions are typically closed with absorbable sutures or adhesive strips.
- Recovery and Follow-up: Following the surgery, you will be monitored in a recovery area until the effects of anaesthesia wear off. Your healthcare team will provide instructions for post-operative care, pain management, and any necessary follow-up appointments.